FDA Approves Ukoniq (umbralisib) for Marginal Zone Lymphoma and Follicular Lymphoma

NEW YORK, Feb. 05, 2021 (GLOBE NEWSWIRE) -- TG Therapeutics, Inc. (NASDAQ: TGTX), today announced the U.S. Food and Drug Administration (FDA) has approved Ukoniq™ (umbralisib), for the treatment of adult patients with relapsed or refractory marginal zone lymphoma (MZL) who have received at least one prior anti-CD20 based regimen and adult patients with relapsed or refractory follicular lymphoma (FL) who have received at least three prior lines of systemic therapy.
Ukoniq is the first and only, oral, once daily, inhibitor of phosphoinositide 3 kinase (PI3K) delta and casein kinase 1 (CK1) epsilon. Accelerated approval was granted for these indications based on overall response rate (ORR) data from the Phase 2 UNITY-NHL Trial (NCT02793583). Continued approval for these indications may be contingent upon verification and description of clinical benefit in a confirmatory trial. This application was granted priority review for the MZL indication. In addition, Ukoniq was granted Breakthrough Therapy Designation (BTD) for the treatment of MZL and orphan drug designation (ODD) for the treatment of MZL and FL.
Michael S. Weiss, Executive Chairman and Chief Executive Officer of TG Therapeutics stated, “Today’s approval of Ukoniq marks a historic day for our Company with this being our first approval and we are extremely pleased to be able to bring our novel inhibitor of PI3K-delta and CK1-epsilon to patients with relapsed/refractory MZL and FL. We have built a commercial team with significant experience who will immediately start to engage our customers to educate them on Ukoniq and how to access the product for patients in need and expect to make Ukoniq available to US distributors in the next few days.” Mr. Weiss continued, “We want to thank the patients, physicians, nurses and clinical coordinators for their support and participation in our clinical trials, and the FDA for their collaboration throughout this process. We remain dedicated to patients with B-cell diseases and our mission of developing treatment options for those in need.”
“Despite treatment advances, MZL and FL remain incurable diseases with limited treatment options for patients who relapse after prior therapy and no defined standard of care. With the approval of umbralisib we now have a targeted, oral, once-daily option, offering a needed treatment alternative for patients,” stated Dr. Nathan Fowler, Professor of Medicine at The University of Texas MD Anderson Cancer Center and the Study Chair of the UNITY-NHL MZL &FL cohorts.
“The approval of umbralisib for the treatment of relapsed/refractory marginal zone lymphoma and follicular lymphoma offers patients a new treatment option, and new hope in the fight against these diseases,” stated Meghan Gutierrez, Chief Executive Officer of the Lymphoma Research Foundation.
EFFICACY & SAFETY DATA IN RELAPSED/REFRACTORY MZL AND FL
The efficacy of Ukoniq monotherapy was evaluated in two single-arm cohorts, within the Phase 2 UNITY-NHL clinical trial, in 69 patients with MZL who received at least 1 prior therapy, including an anti-CD20 regimen, and in 117 patients with FL who received at least 2 prior systemic therapies, including an anti-CD20 monoclonal antibody and an alkylating agent. The UNITY-NHL Phase 2 trial is an open-label, multi-center, multi-cohort study with patients receiving Ukoniq 800 mg once daily. The primary endpoint was independent review committee (IRC) assessed overall response rate (ORR) according to the Revised International Working Group Criteria.
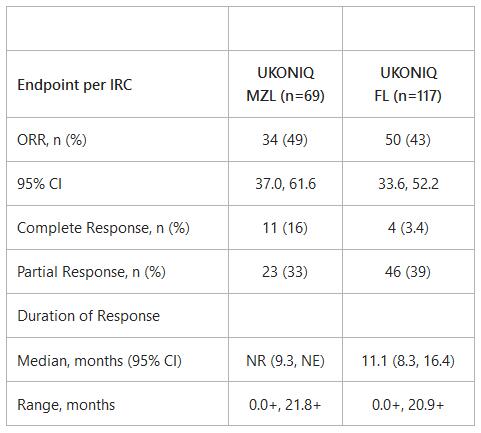
CI, confidence interval; NR, not reached; NE, not evaluable
+Denotes censored observation
The safety of Ukoniq monotherapy was based on a pooled population from the 221 adults with MZL and FL in three single arm, open label trials and one open label extension trial. Patients received Ukoniq 800 mg orally once daily. Serious adverse reactions occurred in 18% of patients who received Ukoniq. Serious adverse reactions that occurred in ≥2% of patients were diarrhea-colitis (4%), pneumonia (3%), sepsis (2%), and urinary tract infection (2%). The most common adverse reactions (>15%), including laboratory abnormalities, were increased creatinine (79%), diarrhea-colitis (58%, 2%), fatigue (41%), nausea (38%), neutropenia (33%), ALT increase (33%), AST increase (32%), musculoskeletal pain (27%), anemia (27%), thrombocytopenia (26%), upper respiratory tract infection (21%), vomiting (21%), abdominal pain (19%), decreased appetite (19%), and rash (18%).
About Ukoniq
Ukoniq is the first and only oral inhibitor of phosphoinositide 3 kinase (PI3K) delta and casein kinase 1 (CK1) epsilon. PI3K-delta is known to play an important role in supporting cell proliferation and survival, cell differentiation, intercellular trafficking and immunity and is expressed in both normal and malignant B-cells. CK1-epsilon is a regulator of oncoprotein translation and has been implicated in the pathogenesis of cancer cells, including lymphoid malignancies.
Ukoniq is indicated for the treatment of adult patients with relapsed or refractory marginal zone lymphoma (MZL) who have received at least one prior anti-CD20-based regimen and for the treatment of adult patients with relapsed or refractory follicular lymphoma (FL) who have received at least three prior lines of systemic therapy.
These indications are approved under accelerated approval based on overall response rate. Continued approval for this indication may be contingent upon verification and description of clinical benefit in a confirmatory trial.
IMPORTANT SAFETY INFORMATION
Infections: Serious, including fatal, infections occurred in patients treated with Ukoniq. Grade 3 or higher infections occurred in 10% of 335 patients, with fatal infections occurring in <1%. The most frequent Grade ≥3 infections included pneumonia, sepsis, and urinary tract infection. Provide prophylaxis for Pneumocystis jirovecii pneumonia (PJP) and consider prophylactic antivirals during treatment with Ukoniq to prevent CMV infection, including CMV reactivation. Monitor for any new or worsening signs and symptoms of infection, including suspected PJP or CMV, during treatment with Ukoniq. For Grade 3 or 4 infection, withhold Ukoniq until infection has resolved. Resume Ukoniq at the same or a reduced dose. Withhold Ukoniq in patients with suspected PJP of any grade and permanently discontinue in patients with confirmed PJP. For clinical CMV infection or viremia, withhold Ukoniq until infection or viremia resolves. If Ukoniq is resumed, administer the same or reduced dose and monitor patients for CMV reactivation by PCR or antigen test at least monthly.
Neutropenia: Serious neutropenia occurred in patients treated with Ukoniq. Grade 3 neutropenia developed in 9% of 335 patients and Grade 4 neutropenia developed in 9%. Monitor neutrophil counts at least every 2 weeks for the first 2 months of Ukoniq and at least weekly in patients with neutrophil count <1 x 109/L (Grade 3-4) neutropenia during treatment with Ukoniq. Consider supportive care as appropriate. Withhold, reduce dose, or discontinue Ukoniq depending on the severity and persistence of neutropenia.
Diarrhea or Non-Infectious Colitis: Serious diarrhea or non-infectious colitis occurred in patients treated with Ukoniq. Any grade diarrhea or colitis occurred in 53% of 335 patients and Grade 3 occurred in 9%. For patients with severe diarrhea (Grade 3, i.e., > 6 stools per day over baseline) or abdominal pain, stool with mucus or blood, change in bowel habits, or peritoneal signs, withhold Ukoniq until resolved and provide supportive care with antidiarrheals or enteric acting steroids as appropriate. Upon resolution, resume Ukoniq at a reduced dose. For recurrent Grade 3 diarrhea or recurrent colitis of any grade, discontinue Ukoniq. Discontinue Ukoniq for life-threatening diarrhea or colitis.
Hepatotoxicity: Serious hepatotoxicity occurred in patients treated with Ukoniq. Grade 3 and 4 transaminase elevations (ALT and/or AST) occurred in 8% and <1%, respectively, in 335 patients. Monitor hepatic function at baseline and during treatment with Ukoniq. For ALT/AST greater than 5 to less than 20 times ULN, withhold Ukoniq until return to less than 3 times ULN, then resume at a reduced dose. For ALT/AST elevation greater than 20 times ULN, discontinue Ukoniq.
Severe Cutaneous Reactions: Severe cutaneous reactions, including a fatal case of exfoliative dermatitis, occurred in patients treated with Ukoniq. Grade 3 cutaneous reactions occurred in 2% of 335 patients and included exfoliative dermatitis, erythema, and rash (primarily maculo-papular). Monitor patients for new or worsening cutaneous reactions. Review all concomitant medications and discontinue any potentially contributing medications. Withhold Ukoniq for severe (Grade 3) cutaneous reactions until resolution. Monitor at least weekly until resolved. Upon resolution, resume Ukoniq at a reduced dose. Discontinue Ukoniq if severe cutaneous reaction does not improve, worsens, or recurs. Discontinue Ukoniq for life-threatening cutaneous reactions or SJS, TEN, or DRESS of any grade. Provide supportive care as appropriate.
Allergic Reactions Due to Inactive Ingredient FD&C Yellow No. 5: Ukoniq contains FD&C Yellow No. 5 (tartrazine), which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons, frequently in patients who also have aspirin hypersensitivity.
Embryo-fetal Toxicity: Based on findings in animals and its mechanism of action, Ukoniq can cause fetal harm when administered to a pregnant woman. Advise pregnant women of the potential risk to a fetus. Advise females and males with female partners of reproductive potential to use effective contraception during treatment and for at least one month after the last dose.
Serious adverse reactions occurred in 18% of 221 patients who received Ukoniq. Serious adverse reactions that occurred in ≥2% of patients were diarrhea-colitis (4%), pneumonia (3%), sepsis (2%), and urinary tract infection (2%). Permanent discontinuation of Ukoniq due to an adverse reaction occurred in 14% of patients. Dose reductions of Ukoniq due to an adverse reaction occurred in 11% of patients. Dosage interruptions of Ukoniq due to an adverse reaction occurred in 43% of patients.
The most common adverse reactions (>15%), including laboratory abnormalities, in 221 patients who received Ukoniq were increased creatinine (79%), diarrhea-colitis (58%, 2%), fatigue (41%), nausea (38%), neutropenia (33%), ALT increase (33%), AST increase (32%), musculoskeletal pain (27%), anemia (27%), thrombocytopenia (26%), upper respiratory tract infection (21%), vomiting (21%), abdominal pain (19%), decreased appetite (19%), and rash (18%).
Lactation: Because of the potential for serious adverse reactions from umbralisib in the breastfed child, advise women not to breastfeed during treatment with Ukoniq and for at least one month after the last dose.
Please visit www.tgtherapeutics.com/prescribing-information/uspi-ukon for full Prescribing Information and Medication Guide.
Physicians, pharmacists, or other healthcare professionals with questions about Ukoniq should visit www.UKONIQ.com.
ABOUT TG PATIENT SUPPORT
The TG Patient Support is a comprehensive program designed by TG Therapeutics to support patients through their treatment journey and the reimbursement process. More information about the TG Patient Support program is accessible by phone at 1-877-TGTXPSP (1-877-848-9777); by fax at 1-877-778-1329 or at www.UKONIQ.com/patient/patientsupport.
ABOUT MARGINAL ZONE LYMPHOMA
Marginal zone lymphoma (MZL) comprises a group of indolent (slow growing) mature B-cell non-Hodgkin lymphomas (NHLs). MZL is generally considered a chronic and incurable disease. With an annual incidence of approximately 8,200 newly diagnosed patients in the United States1,2, MZL is the third most common B-cell NHL, accounting for approximately ten percent of all NHL cases. MZL consists of three different subtypes: extranodal MZL of the mucosal-associated lymphoid tissue (MALT), nodal marginal zone lymphoma (NMZL), and splenic marginal zone lymphoma (SMZL)3.
ABOUT FOLLICULAR LYMPHOMA
Follicular lymphoma (FL) is typically an indolent form of non-Hodgkin lymphoma (NHL) that arises from B-lymphocytes. It is the second most common form of NHL. FL is generally not curable and is considered a chronic disease, as patients can live for many years with this form of lymphoma. With an annual incidence in the United States of approximately 13,200 newly diagnosed patients1,2, FL is the most common indolent lymphoma accounting for approximately 17 percent of all NHL cases4.
ABOUT TG THERAPEUTICS, INC.
TG Therapeutics is a fully-integrated, commercial stage biopharmaceutical company focused on the acquisition, development and commercialization of novel treatments for B-cell malignancies and autoimmune diseases. In addition to an active research pipeline including five investigational medicines across these therapeutic areas, TG has received accelerated approval from the U.S. FDA for Ukoniq (umbralisib), for the treatment of adult patients with relapsed/refractory marginal zone lymphoma who have received at least one prior anti-CD20-based regimen and relapsed/refractory follicular lymphoma who have received at least three prior lines of systemic therapies. Currently, the Company has two programs in Phase 3 development for the treatment of patients with relapsing forms of multiple sclerosis (RMS) and patients with chronic lymphocytic leukemia (CLL) and several investigational medicines in Phase 1 clinical development. For more information, visit www.tgtherapeutics.com, and follow us on Twitter @TGTherapeutics and Linkedin.
Ukoniq is a registered trademark of TG Therapeutics, Inc.
1National Cancer Institute. SEER Cancer Statistics Review 2008-2017: Non-Hodgkin Lymphoma. Table 19.26. https://seer.cancer.gov/csr/1975_2017/results_single/sect_19_table.26_2pgs.pdf. Accessed January 19, 2021.
2National Cancer Institute. SEER Cancer Stat Facts: Non-Hodgkin Lymphoma. https://seer.cancer.gov/statfacts/html/nhl.html. Accessed January 19, 2021.
3 Lymphoma Research Foundation: Marginal Zone Lymphoma
https://lymphoma.org/aboutlymphoma/nhl/mzl/
4 Lymphoma Research Foundation “Follicular Lymphoma”
Source: TG Therapeutics, Inc.
Posted: February 2021

