Complete Results from Second Pivotal Monotherapy Study of Abrocitinib Published in JAMA Dermatology
NEW YORK--(BUSINESS WIRE) June 03, 2020 -- Pfizer Inc. (NYSE: PFE) announced today that JAMA Dermatology has published complete results from the second Phase 3 monotherapy pivotal study (JADE MONO-2) of abrocitinib, an investigational oral once-daily Janus kinase 1 (JAK1) inhibitor, in patients aged 12 and older with moderate to severe atopic dermatitis (AD). Consistent with the first Phase 3 monotherapy study (JADE MONO-1), both doses of abrocitinib met all co-primary and key secondary endpoints and were generally well tolerated.
“Results from the second pivotal trial for abrocitinib reinforce the potential symptom relief it can offer those living with moderate to severe atopic dermatitis, including for itch — one of the most bothersome symptoms of AD,” said Michael Corbo, PhD, Chief Development Officer, Inflammation & Immunology, Pfizer Global Product Development. “We are hopeful that these findings, should abrocitinib be approved, will translate into meaningful improvements for patients who face daily challenges with this disease.”
JADE MONO-2 Trial Design
JADE MONO-2 was a randomized, double-blind, placebo-controlled, parallel-group study designed to evaluate the efficacy and safety of two doses (100mg and 200mg once daily) of abrocitinib monotherapy over 12 weeks. A total of 391 subjects with moderate to severe atopic dermatitis were randomized to abrocitinib 200mg, abrocitinib 100mg, and placebo in the trial.
Efficacy endpoints evaluated measures of improvements in skin clearance, disease extent and severity, and itch. The co-primary study endpoints in JADE MONO-2 were the proportion of patients who achieved:
an Investigator Global Assessment (IGA) score of clear (0) or almost clear (1) skin and two-point or greater improvement relative to baseline at Week 12.
at least a 75% or greater change from baseline in their Eczema Area and Severity Index (EASI) score at Week 12.
The key secondary endpoint was the proportion of patients achieving a four-point or larger reduction in itch severity measured with the Peak Pruritus Numerical Rating Scale (PP-NRS) at Weeks 2, 4, and 12. The proportion of patients who achieved a 90% or greater change from baseline in EASI score at Week 12 was included as a secondary endpoint.
JADE MONO-2 Study Efficacy Results1
By Week 12, a greater proportion of patients on either dose of abrocitinib achieved the IGA, EASI-75, PP-NRS, and EASI-90 responses compared to those on placebo. The following co-primary efficacy and secondary endpoint results were seen at Week 12:
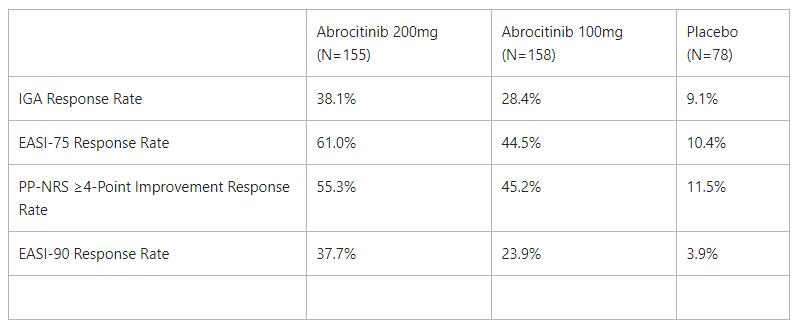
The proportion of patients achieving the IGA, EASI-75, PP-NRS, and EASI-90 responses were higher for abrocitinib treatment at each time point compared with placebo from Week 2 to Week 12, with responses seen as early as Week 2. Similar to JADE MONO 1, significant IGA, EASI-75, and PP-NRS responses were observed from Week 2 through Week 12.
JADE MONO-2 Study Safety Results1
The most frequently reported treatment-emergent adverse events were nausea, nasopharyngitis, and atopic dermatitis in the abrocitinib 200mg, abrocitinib 100mg, and placebo groups, respectively.
Observed serious adverse events that were considered related to treatment were reported for two patients in the abrocitinib 100mg group (herpangina and pneumonia) and one patient with two events in the placebo group (eczema herpeticum and staphylococcal infection). There were no serious treatment-related adverse events in the 200mg group.
One patient with co-existing cardiovascular risk factors died from unknown etiology three weeks after receiving the last dose of abrocitinib 100mg once daily, which was deemed unrelated to the study drug by the investigator.
Other safety findings included:
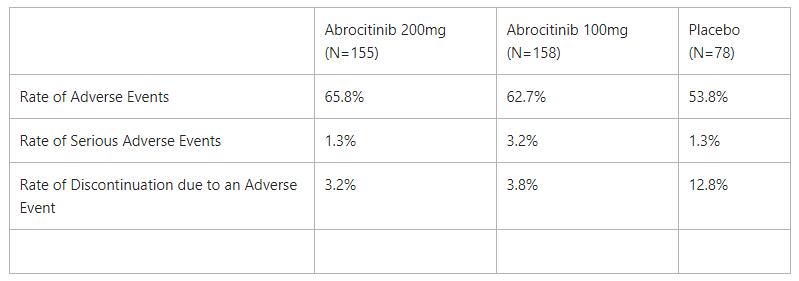
The most frequently reported AEs leading to treatment discontinuation were headache in the abrocitinib 200mg group and atopic dermatitis in the abrocitinib 100mg and the placebo groups.
Additional Details About the JADE MONO-2 Study
Randomization was stratified by baseline disease severity (moderate [IGA=3] and severe [IGA=4] AD) and age (age <18 and ≥18 years). Concomitant use of topical or systemic therapies for AD or rescue medication was not permitted. Patients were permitted to use oral antihistamines and topical non-medicated emollients during the study. Eligible subjects completing the 12-week treatment period of the study had the option to enter a long-term extension (LTE) study, B7451015. Subjects discontinuing early from treatment, or who were otherwise ineligible for the LTE study, entered a 4-week follow up period in this study.
JADE MONO-2 is the second trial in the JAK1 Atopic Dermatitis Efficacy and Safety (JADE) global development program. Pfizer recently announced positive top-line results from the third trial in the program, JADE COMPARE. Additional data from other studies in the JADE program will be available later this year.
For additional information about JADE MONO-2, please visit https://www.clinicaltrials.gov.
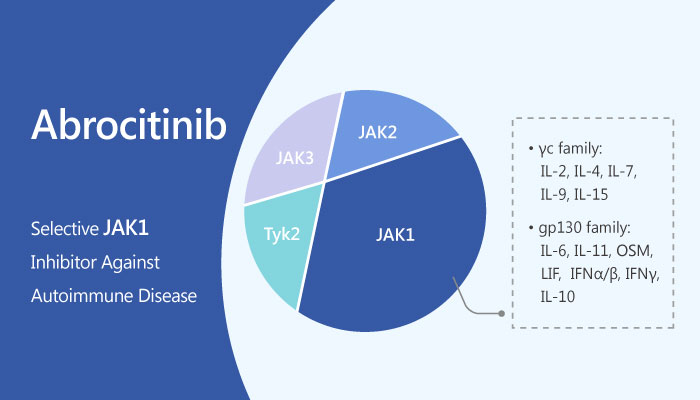
About Abrocitinib
Abrocitinib is an oral small molecule that selectively inhibits Janus kinase (JAK) 1. Inhibition of JAK1 is thought to modulate multiple cytokines involved in pathophysiology of atopic dermatitis, including interleukin (IL)-4, IL-13, IL-31, IL-22 and thymic stromal lymphopoietin (TSLP).
Abrocitinib received Breakthrough Therapy designation from the FDA for the treatment of patients with moderate to severe AD in February 2018. Breakthrough Therapy designation was initiated as part of the Food and Drug Administration Safety and Innovation Act (FDASIA) signed in 2012. As defined by the FDA, a breakthrough therapy is a drug intended to be used alone or in combination with one or more other drugs to treat a serious or life-threatening disease or condition, and preliminary clinical evidence indicates that the drug may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints, such as substantial treatment effects observed early in clinical development. If a drug is designated as a Breakthrough Therapy, the FDA will expedite the development and review of such drug.2
About Atopic Dermatitis
AD is a chronic skin disease characterized by inflammation of the skin and skin barrier defects.3,4 Lesions of AD are characterized by erythema (redness), itching, induration (hardening)/papulation (formulation of papules), and oozing/crusting.3,4
AD is one of the most common, chronic, relapsing childhood dermatoses, affecting up to 10% of adults and up to 20% of children worldwide.5,6
About Pfizer’s Immunokinase Inhibitor Leadership
The JAK pathways are believed to play an important role in inflammatory processes as they are involved in signaling for over 50 cytokines and growth factors, many of which drive immune-mediated conditions.7 JAK inhibition may offer patients with these conditions a potential new advanced treatment option.8
Pfizer’s leading JAK biology and chemistry expertise combined with our research experience, has uniquely enabled the company to take a different R&D approach to that of other companies involved in JAK research, resulting in one of the broadest immunokinase inhibitor pipelines. Instead of studying a single molecule for all its potential uses, where it may not be optimal for some, Pfizer’s candidates with unique selectivity profiles are purposefully matched to the conditions where we believe they have the greatest potential to, if approved, address unmet need. Pfizer has five unique immunokinase inhibitors in late-stage clinical trials for the potential treatment of ten immune-mediated diseases:
Abrocitinib: A JAK1 inhibitor in phase 3 clinical trials for the potential treatment of moderate-to-severe AD among adolescents and adults
PF-06651600: An oral, JAK3/TEC family kinase inhibitor in a phase 3 clinical trial for the potential treatment of alopecia areata (AA) and in phase 2 for vitiligo, Crohn’s disease (CD), and ulcerative colitis (UC)
PF-06700841: A tyrosine kinase 2(TYK2)/JAK1 inhibitor in phase 2 clinical trials for the potential treatment of psoriasis and AD in topical formulation, and, in oral formulation for psoriatic arthritis, CD, UC, vitiligo, systemic lupus erythematosus (SLE), AA and hidradenitis suppurativa (HS)
PF-06826647: A TYK2 inhibitor under investigation in phase 2 clinical trials for the potential treatment of psoriasis and HS
PF-06650833: An IL-1 receptor associated kinase 4 (IRAK4) inhibitor under investigation for the potential treatment of rheumatoid arthritis and HS in phase 2 clinical trials
Pfizer Inc.: Breakthroughs that Change Patients’ Lives
At Pfizer, we apply science and our global resources to bring therapies to people that extend and significantly improve their lives. We strive to set the standard for quality, safety and value in the discovery, development and manufacture of health care products, including innovative medicines and vaccines. Every day, Pfizer colleagues work across developed and emerging markets to advance wellness, prevention, treatments and cures that challenge the most feared diseases of our time. Consistent with our responsibility as one of the world's premier innovative biopharmaceutical companies, we collaborate with health care providers, governments and local communities to support and expand access to reliable, affordable health care around the world. For more than 150 years, we have worked to make a difference for all who rely on us. We routinely post information that may be important to investors on our website at www.pfizer.com. In addition, to learn more, please visit us on www.pfizer.com and follow us on Twitter at @Pfizer and @Pfizer_News, LinkedIn, YouTube and like us on Facebook at Facebook.com/Pfizer.
A further description of risks and uncertainties can be found in Pfizer’s Annual Report on Form 10-K for the fiscal year ended December 31, 2019 and in its subsequent reports on Form 10-Q, including in the sections thereof captioned “Risk Factors” and “Forward-Looking Information and Factors That May Affect Future Results”, as well as in its subsequent reports on Form 8-K, all of which are filed with the U.S. Securities and Exchange Commission and available at www.sec.gov and www.pfizer.com.
1 Silverberg JI, Simpson EL, Thyssen JP, et al. Efficacy and Safety of Abrocitinib in Patients With Moderate-to-Severe Atopic Dermatitis: A Randomized Clinical Trial. JAMA Dermatol. Published online June 03, 2020. doi:10.1001/jamadermatol.2020.1406.
2 U.S. Food and Drug Administration. Fact Sheet: Breakthrough Therapies at https://www.fda.gov/RegulatoryInformation/LawsEnforcedbyFDA/SignificantA... accessed on August 16, 2019.
3 Hanifin JM, Reed ML. A population-based survey of eczema in the United States. Dermatitis. 2007;18(2):82-91.
4 Bieber T. Atopic dermatitis. Dermatology. 2012;1(3):203-217.
5 Oszukowska M, Michalak I, Gutfreund K, et al. Role of primary and secondary prevention in atopic dermatitis. Postep Derm Alergol. 2015:32(6):409-420.
6 Nutten S. Atopic dermatitis: global epidemiology and risk factors. Ann Nutr Metab. 2015;66(suppl 1):8-16.
7 Banerjee, S., Biehl, A., Gadina, M. et al. JAK–STAT Signaling as a Target for Inflammatory and Autoimmune Diseases: Current and Future Prospects. Drugs. 2017;77: 521. https://doi.org/10.1007/s40265-017-0701-9.
8 Telliez JB, Dowty ME, Wang L, Jussif J, Lin T, Li L, et al. Discovery of a JAK3-selective inhibitor: functional differentiation of JAK3-selective inhibition over pan-JAK or JAK1-selective inhibition. ACS Chem Biol. 2016;11(12):3442–51. doi:10.1021/acschembio.6b00677.
Source: Pfizer Inc.
Posted: June 2020

